Prostate Cancer Treatment Information
Prostate cancer is the most frequently diagnosed malignancy in American men (aside from skin cancer), and it is especially common after age 50. The cancer occurs when cells in or around the prostate—a walnut-sized gland that produces seminal fluid—undergo abnormal changes that cause them to grow and divide uncontrollably. The excess cells then bind together and form a tumor.
In many cases, prostate cancer is relatively slow-growing, which means that it can take several years to become large enough to be detected, and even longer to grow and spread outside the prostate. However, some cases are more aggressive and require more urgent treatment.
What causes prostate cancer?
Advanced age is the primary risk factor for prostate cancer, followed by a family history of prostate, breast, ovarian, colon or pancreatic cancer. Certain lifestyle factors, such as tobacco use, obesity and poor nutrition, also seem to play a role in its development. However, an unhealthy lifestyle is associated with many health issues that can change the course of any illness, including prostate cancer.
Within the general medical community, the precise causes of prostate cancer are not yet well understood. Researchers are currently studying specific genetic and lifestyle factors to determine whether (and to what extent) those factors contribute to its development.
What are the symptoms of prostate cancer?
In most cases, prostate cancer is silent. Due to the location of the prostate gland deep within the groin, a growing tumor would not be close enough to painfully press on any nearby organs or tissues. With that said, some men experience:
- Burning sensations during urination
- Difficulty starting and stopping urination
- A weak urine stream
- More frequent urination, especially at night
- Bloody urine
- Pain during ejaculation
- Bloody semen
More often, the cause of these symptoms is unrelated to prostate cancer, so it’s important to discuss them with a physician before drawing any conclusions. As part of the diagnostic process, a physician may perform a digital rectum exam (DRE) to manually check the prostate and order a prostate-specific antigen (PSA) test to measure the level of PSA (a protein produced by the prostate) in the blood.
Although an elevated PSA level may be a sign of prostate cancer, it could also indicate a noncancerous condition, such as prostate inflammation (prostatitis) or enlargement (benign prostatic hyperplasia). Therefore, if a PSA test reveals an elevated PSA level, a physician will typically order a biopsy to confirm or rule out a diagnosis of prostate cancer.

Rated High Performing in Prostate Cancer Surgery
Schedule an AppointmentWhat are the types of prostate cancer?
The most common type of prostate cancer, diagnosed in nearly all cases, is prostatic adenocarcinomas. All other prostate cancer types comprise an estimated 1-5% of cases. Prostatic adenocarcinoma develops in the glandular epithelial cells that line the prostate and can be categorized into two subtypes:
- Acinar adenocarcinoma – Most prostate cancers are diagnosed as acinar adenocarcinomas. It produces elevated PSA levels and, since the cells grow in the back of the prostate near the rectum, the cancerous cells can sometimes be felt during a digital rectal exam, making this subtype easier to detect.
- Prostatic ductal adenocarcinoma – A rarer, more aggressive form of prostatic adenocarcinoma, this subtype develops in the cells lining the tubes and ducts of the prostate gland. It’s harder to detect and often develops alongside acinar adenocarcinoma.
Other, less common types of prostate cancer include urothelial cancer, neuroendocrine tumors, small cell carcinoma, squamous cell carcinoma and soft-tissue prostate cancer.
How is prostate cancer treated?
In most cases, prostate cancer is highly responsive to treatment. Additionally, because the cancerous cells typically grow very slowly, some men are candidates for active surveillance, which involves delaying treatment and instead opting for a structured program of periodic PSA tests, advanced imaging scans and biopsies to monitor the tumor.
The goal of prostate cancer treatment is to achieve the most favorable outcome while minimizing side effects, preserving prostate function and ensuring the best possible quality of life. Some options include:
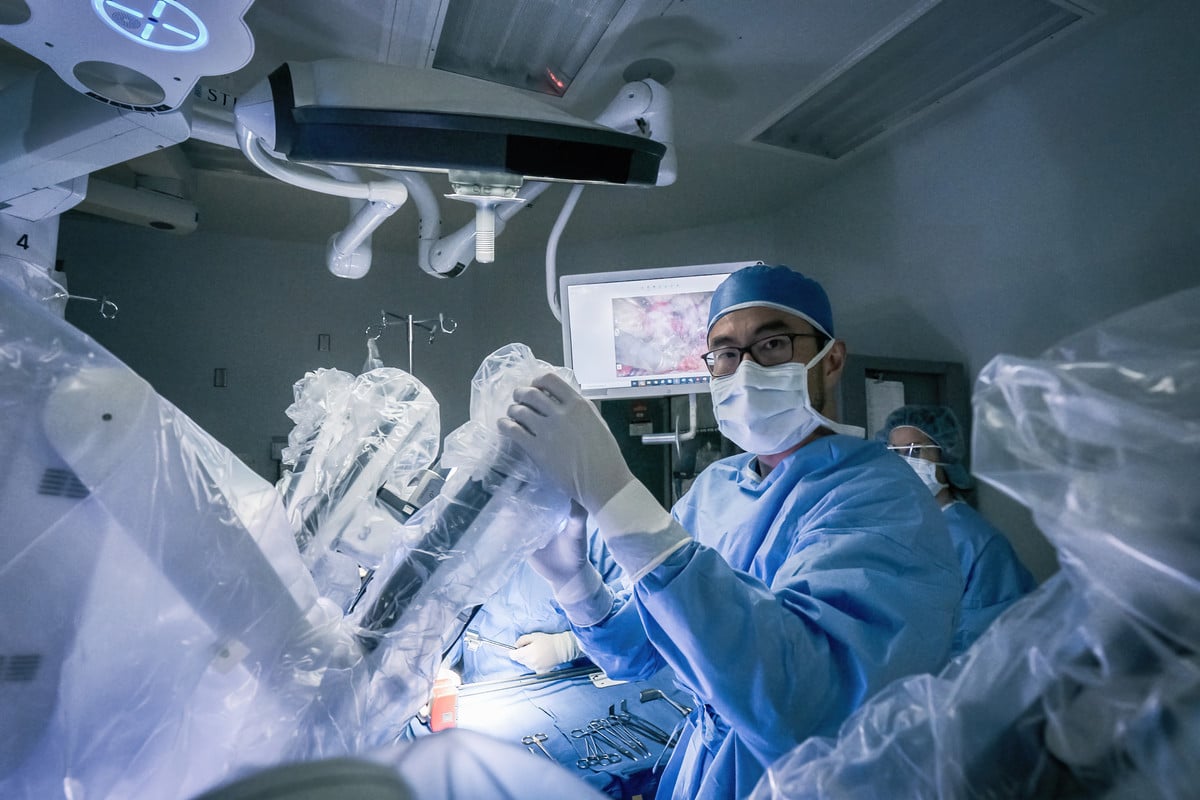
Surgery
A surgical procedure known as a radical prostatectomy, which involves the removal of the entire prostate along with some nearby lymph nodes, is a common option for addressing cancer that has not spread beyond the prostate. In addition to the traditional open approach, a surgeon may perform this surgery utilizing minimally invasive techniques and/or robotic assistance, which can result in a quicker recovery.
Radiation therapy
To treat prostate cancer, radiation therapy may be delivered externally or internally. External beam radiation involves the use of a linear accelerator, which generates high-energy rays and sends them directly to the tumor site. Internal radiation therapy (brachytherapy) involves the placement of tiny radioactive pellets in or near a prostate tumor.
Chemotherapy
A systemic treatment, chemotherapy may be used to target cancerous cells that have spread from the prostate to distant areas of the body. After being administered orally or intravenously, powerful drugs enter the bloodstream, then circulate throughout the body to reach and destroy rapidly dividing cells.
Immunotherapies
Immunotherapies do not directly target prostate cancer, but rather work by stimulating the body’s immune system to help it fight the malignancy. Provenge® is a cancer vaccine that has received approval from the U.S. Food and Drug Administration (FDA) for use as an immunotherapy for advanced prostate cancer. This customized treatment uses the patient’s own immune cells, which are exposed to a specific protein that improves their ability to identify and target prostate cancer cells.
Moffitt’s approach to prostate cancer treatment
Having earned the prestigious Comprehensive Cancer Center designation from the National Cancer Institute (NCI), Moffitt Cancer Center has distinguished itself as one of the nation’s premier cancer centers. Through our extensive research, bench-to-bedside approach and robust clinical trials program, our patients have opportunities to be among the first to benefit from promising new prostate cancer treatments that are unavailable elsewhere.
The renowned Urologic Oncology Program at Moffitt features a multispecialty team that includes board-certified surgeons, radiologists, radiation oncologists, nurses, supportive care specialists and other medical professionals. Working together, these diverse experts develop a tailored treatment plan for each patient. Moffitt also holds weekly tumor board meetings to assess and monitor complex cases. These are just some of the ways in which we provide outstanding cancer care.
If you have a high PSA level and require further testing, you can be screened for prostate cancer at Moffitt. No referral needed. Or, if you would like more information about prostate cancer, you are welcome to talk with a specialist in the Urologic Oncology Program at Moffitt Cancer Center. To request an appointment, please call 1-888-663-3488 or submit a new patient registration form online.



