Clinical Trials Give Anaplastic Thyroid Cancer Patients a Fighting Chance
June Perez wakes up every morning at 6:30 to have her daily prayer time. It serves as a time to reflect and be thankful for everything life has given her. One morning in March 2018, she woke up to go through her usual prayer routine but discovered something unusual. A marble-sized lump had appeared in her neck. Less than two hours later the lump had doubled in size and she knew something was wrong. She saw her doctor a few hours later and the lump had gown even more.
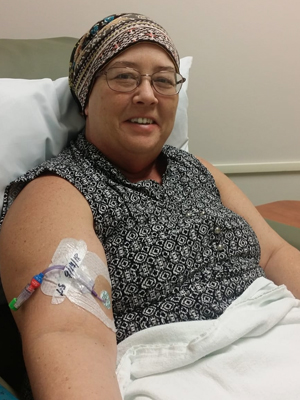
June Perez was diagnosed with anaplastic thyroid cancer in 2018.
“It was really growing almost in front of me,” said Perez. “So my doctor sent me for an ultrasound and later that day they said, ‘We think you have a tumor on your thyroid.’”
Her first biopsy was inconclusive. Appointments with endocrinologists and other specialists held few answers. A surgeon told her that “maybe” she had thyroid cancer, but even if she did, she was assured it would be very treatable and was nothing to worry about.
Dr. Bryan McIver, deputy physician-in-chief at Moffitt Cancer Center and senior member in the Endocrine Oncology Program, doesn’t buy into the mantra that thyroid cancer is a “good” type of cancer to be diagnosed with.
“Thyroid cancer is a remarkable beast,” said McIver. “In most patients we can catch the cancer relatively early and the treatment outcomes are usually excellent. They tend to be slow growing, slow to spread and slow to invade, so the general kind of feeling about thyroid cancer is that it’s a ‘good’ cancer, but I think that’s completely wrong. There is no such thing as a ‘good cancer’!”
A Beast for Older Patients
Thyroid cancer is commonly diagnosed at a younger age than most other adult cancers, which contributes to the high rates of successful treatment. But it is in the older patient population where thyroid cancer can become the beast.
“Once you’re in your 50s or 60s, the type of thyroid cancer we see has a tendency to be more aggressive than the same cancer in younger people,” said McIver. “So often we see cancers that are more likely to invade, more likely to spread and more likely to create problems. The worst of the worst is anaplastic thyroid cancer.”

According to McIver, anaplastic thyroid cancer is one of the most aggressive types of cancers. While rare, only accounting for around 2% of all thyroid cancers, it’s survivability is comparable to pancreatic and lung cancers, which are widely considered among the deadliest forms of cancer.
Perez was 58 when she found the lump in her neck. When a surgeon went in for a closer look, her diagnosis became clear. It was anaplastic thyroid cancer.
“My surgeon was in tears,” said Perez. “Just sharing that there’s really nothing that we know to do. The prognosis was really bad.”
Perez tried to schedule follow-up appointments, but knew the clock was ticking. Without a clear treatment plan, she took her health into her own hands.
“My doctor just said that the best thing for me to do is find a place that will offer clinical trials,” said Perez. “But he just basically sent me home. So I went home and I looked up clinical trials and found Moffitt.”
After one email, Perez was set up with an appointment to see McIver the following day. If she hadn’t taken action, it would have been weeks before another specialist could see her.
“Dr. McIver called a tumor board together that day while we were still in the clinic,” said Perez. “By the time I left, we had a plan and a week later I had surgery to have the tumor removed.”
Dr. Kristen Otto, a surgeon in Moffitt’s Endocrine Oncology Program, removed the tumor that had invaded Perez’s vocal cords, trachea and jugular vein. Following surgery, Perez began chemotherapy and radiation treatments. By October she had begun her first of three clinical trials.
“It meant everything just being able to try something to fight this cancer after being told by previous doctors, ‘we don’t know how to treat this,’” said Perez. “Just seeing the doctors that I had at Moffitt really fighting for me and, trying to find something that was a good fit and feeling like they’ve studied it enough to know what might work felt like they were really trying to be a fighter on my side. It was just what I needed at that moment because that’s a devastating diagnosis.”
Targeted Therapy Improving Survival
According to McIver, about 10 years ago there were no known treatments for anaplastic thyroid cancer. A decade ago Perez likely would have been told to go home and get her affairs in order.
“In the past decade we’ve learned that we can improve outcomes with aggressive surgery, radiation treatment and chemotherapy,” said Mciver. “But much more recently we have learned that targeted treatments towards cancers with specific genetic mutations, known as BRAF mutations, has shown improved survival rates in the subset of patients with that specific mutation.”
Perez did not have a BRAF mutation, so targeted therapy wasn’t an option. While surgery, radiation and chemotherapy did get the cancer in her neck under control temporarily, test results soon showed that her cancer had spread to her lungs.
“That is typically the death knell at that point,” said McIver. “But we were very fortunate to have a clinical trial that we were able to get her into and the outcome has been a spectacular success.”
By October 2019, less than two years after waking up and finding that lump in her neck, Perez had no evidence of disease.

Perez had no evidence of disease less than two years after her initial diagnosis.
“It was really a miracle,” said Perez. “I know it was the trial and I know it was the doctors and the surgeons and the hematologists and the pharmacists and everybody I met at Moffitt just fighting hard to get me the best treatment they thought I could have. It was a really hard thing to go through, but a great experience to have somebody advocate for your health like that and not just throw their hands up in the air and say, ‘I don't know’ and that’s my story.”
For McIver, Perez’s ability to keep fighting feels like a personal victory over a deadly disease that he’s worked to fight for the past 35 years.
“We say the word ‘courage’ a lot when we’re treating patients with cancer,” McIver said. “Ms. Perez exemplifies that courage. She battled this disease. She fought it. I can’t say enough about her determination. She pulled through. To have someone like her survive this is incredibly gratifying. It’s a reminder to us about the importance of research — including clinical trials — that has been going on for years in an effort to improve our ability to treat diseases like this. And it’s a reminder, too, to never give up without a fight!”



