Surgery Can Prevent Pancreatic Cancer in Some Patients
Avia Sutherland was expecting to just see kidney stones on her scan. Instead, doctors found pancreatic cysts.
She didn’t think much of it—most pancreatic cysts are noncancerous—but her doctor urged her to set up an appointment at Moffitt Cancer Center’s Gastrointestinal Oncology Clinic. There, a more in-depth work-up showed although Sutherland didn’t have pancreatic cancer, she did have intraductal papillary mucinous neoplasms (IPMN) with high risk features. If left untreated, IPMN can progress to invasive pancreatic cancer.
While there is no screening for pancreatic cancer, there has been an increase in finding pancreatic cysts in patients. This is credited to a greater use of x-rays and technological advancements, as most cysts are found during unrelated scans.
Pancreatic cancer has the lowest five-year survival rate of any cancer, and by 2020 it will most likely be the number two cause of all cancer-related deaths after lung cancer. But for some, like Sutherland, there is an opportunity to try to prevent the deadly disease.
Sutherland’s surgeon, Dr. Pamela Hodul, recommended Sutherland for a total pancreatectomy, which is the removal of the pancreas. In many of these cases, surgeons also remove the patient’s spleen.
The complicated surgery isn’t for everyone; Moffitt surgeons only performs about 10 to 20 total pancreatectomies a year, and patients who are eligible for the surgery have to fulfill specific criteria. “In the absence of cancer, patients must have diffuse IPMN of the main duct and/or the side branches, along with high-risk features,” said Hodul. “A high-risk feature could be a strong family history of the disease.”
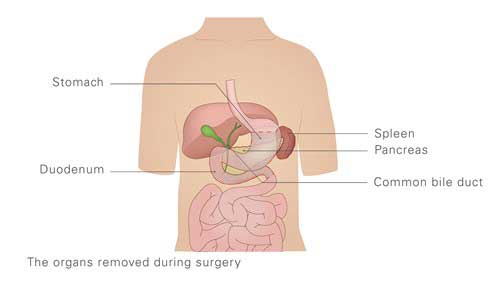
The diagram above depicts the organs removed during a total pancreatectomy procedure.
Patients who undergo a pancreatectomy will also have life-long changes to their health. Without a pancreas, patients become a Type 1 diabetic. On top of giving themselves insulin, they will also need pancreatic enzyme replacement therapy to help with digestion.
“We provide pre-operative consultations and a lot of post-operative education,” said Hodul. “There is a learning curve, but the majority of patients go on to live healthy lifestyles like other diabetics.”
That’s what Sutherland is doing now. Since her life-saving pancreatectomy in 2016, she says she feels great. “I think if I didn’t have the surgery, I would be battling pancreatic cancer right now,” she said. “Naturally, I felt uncomfortable after the surgery, but it didn’t stop me. I feel fantastic and I still do a lot of things at 81 years old.”
One of the most important things Sutherland had after surgery was a support system. Her daughter, who is a nurse, has been with her every step of the way. Sutherland says she is now comfortable with her new routine, and it hasn’t stopped her from traveling and visiting friends and family.