What Is Personalized Medicine?
No two people are exactly the same, so why would medical care be? Personalized, or precision, medicine tailors prevention, diagnosis and treatment to an individual person rather than using a one-size-fits-all approach.
It plays a major role in cancer care because while the disease may look the same under a microscope, it can act differently in each patient. Personalized medicine includes using genetic sequencing to identify cancer mutations, administering targeted therapies and immunotherapies and adjusting treatment based on disease response.

Personalized medicine is transforming cancer treatment, particularly in immunotherapy, where understanding a patient’s tumor biology and immune response is critical, said Kedar Kirtane, MD, the medical director for Solid Tumor Cellular Therapy at Moffitt Cancer Center. “Moffitt is a leader in this space, translating scientific discovery into individualized therapies that improve outcomes for patients.”
Biomarker Testing
The Moffitt STAR (Solid Tumor Actionable Result) 2.0 panel is an all-in-one test that uses a small amount of tissue to examine 517 genes that are commonly involved in cell growth. The test evaluates both DNA and RNA to detect any types of gene changes in a tumor that could be targeted by specific treatment.
The RNA STEP is a complementary expression test that can help match patients to certain clinical trials, and the Safire X (Solid Tumor Archer Fusion Integrated RNA Extended) test can rapidly test 141 genes, which is especially helpful for sarcoma and head and neck cancer diagnoses.
Genetic Testing
Pharmacogenomics is the study of how your genes affect the way your body responds to medicines. In cancer care, it is used to make cancer treatment safer and more effective by matching drugs and doses to a patient’s genetics. For example, some chemotherapy drugs may linger longer in patients with slow-metabolizing genes, or certain hormone therapies may be ineffective in patients who can’t metabolize them properly. Genetic testing can help avoid wasting time on treatments unlikely to work.
Targeted Therapies
Targeted therapies are designed to attack specific mutations in cancer cells while sparing the surrounding healthy cells. They typically target specific proteins that help cancer cells divide and grow. The treatments can lead to fewer side effects, better quality of life and in some cases improved survival outcomes. For example, there are therapies that target the HER2 protein in HER2-positive breast cancer and therapies that target the BRAF protein in BRAF-mutated melanoma.
Immunotherapy
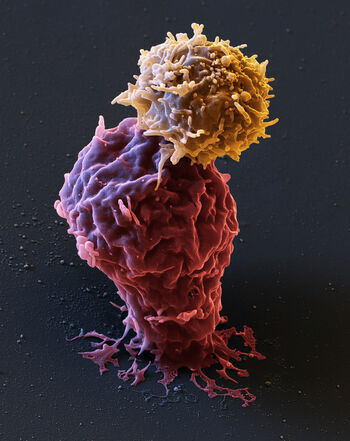
A CAR T cell (orange) attacks a leukemia cancer cell (red).
Personalized medicine can help predict who will respond to immunotherapy, which boosts the immune system to fight cancer. Doctors can test for certain things, such as PD-L1 expression, that can indicate if a certain immunotherapy is more likely to work.
Checkpoint inhibitors are a type of immunotherapy that targets immune checkpoints. They release the brakes on the immune system to encourage it to attack cancer. They are used in many different types of cancer, including bladder, breast and lung cancers, melanoma and Hodgkin lymphoma.
Cellular immunotherapies, such as CAR T-cell therapy and tumor infiltrating lymphocyte (TIL) therapy, are also a highly personalized form of medicine. Both involve genetically engineering a patient’s own immune cells to recognize and attack cancer cells.




