Breast Reconstruction Surgery
Breast reconstruction surgery is an option for individuals who undergo mastectomy or lumpectomy as part of breast cancer treatment. The procedure can be performed immediately during cancer surgery or scheduled for a later time, depending on the treatment plan and personal preferences. Advances in surgical techniques allow many patients to choose a reconstruction approach that aligns with both their medical needs and aesthetic goals.
Regardless of when it takes place, breast reconstruction can be an important part of the recovery process, helping restore the natural appearance of the breast and supporting confidence and overall sense of well-being.
What is the Difference Between Immediate and Delayed Breast Reconstruction?
The difference between immediate and delayed breast reconstruction is when the procedure is performed. Immediate reconstruction is performed at the same time as the mastectomy or lumpectomy. Delayed reconstruction is performed weeks, months or even years after cancer surgery, often after treatments such as chemotherapy or radiation therapy have been completed.
Immediate Breast Reconstruction
Immediate breast reconstruction is performed during the same operation as the cancer-removal surgery. Because the breast shape is rebuilt right away, this approach can help preserve the natural skin envelope and may reduce the total number of surgeries.
Potential benefits may include:
- Fewer total surgical procedures
- Improved cosmetic outcomes
- Psychological benefit of waking up with a reconstructed breast
However, immediate reconstruction may not be recommended for all patients. If radiation therapy is planned, surgeons may recommend delaying reconstruction to reduce the risk of complications.
Oncoplastic surgery, which combines lumpectomy and reconstruction in the same operation, is considered a form of immediate reconstruction.

"Although we understood the severity of what I was dealing with, Dr. Susan Hoover promised and assured me that I was going to be on the other side of cancer in two years."
Tiffany, Breast Cancer Survivor
Request an AppointmentDelayed Breast Reconstruction
Delayed breast reconstruction is performed after the initial cancer surgery has healed. It may take place months or years later, depending on the patient’s treatment plan and recovery. This allows the body to fully heal and cancer treatments to be completed before reconstruction is performed.
This approach may be recommended for patients who:
- Require radiation therapy
- Prefer to focus first on cancer treatment
- Need additional time to consider reconstruction options
Delayed reconstruction can still achieve natural-looking results and remains an option even many years after a mastectomy.
A multidisciplinary breast cancer team, including surgical oncologists and reconstructive specialists, can help determine the most appropriate timing based on the patient’s diagnosis, treatment plan and personal preferences.
The comparison below highlights how timing, recovery and treatment coordination may differ between the two approaches.
| Immediate Reconstruction |
Delayed Reconstruction |
| Performed during cancer surgery | Performed after healing or treatment |
| May preserve more natural skin | Allows time for radiation therapy |
| May reduce total surgeries | Greater flexibility in timing |
| Not suitable for all patients | Can be done months or years later |
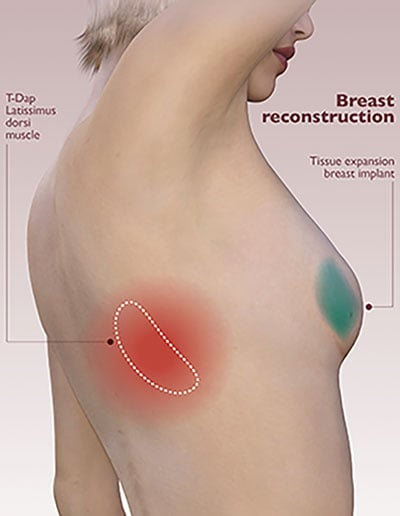
What are The Types of Breast Reconstruction Surgery?
There are two main types of breast reconstruction surgery: implant-based reconstruction and autologous (flap) reconstruction, which uses the patient’s own tissue. The right option depends on individual anatomy, the cancer treatment plan, the need for radiation therapy, and personal goals.
Implant-Based Reconstruction
Implant-based reconstruction is the most common type of breast reconstruction. It uses a saline or silicone implant to recreate the shape of the breast after a mastectomy. This approach does not require tissue from another part of the body and is typically less invasive than flap reconstruction. It can be performed either in stages or, in some cases, as a direct-to-implant procedure.
Tissue Expander and Implant Reconstruction
After a mastectomy, a surgeon may place a tissue expander beneath the chest muscle. This temporary device contains a small valve and is gradually filled with saline over several weeks or months to stretch the skin and create space for a permanent implant. Once the tissue has expanded sufficiently, a second procedure is performed to remove the expander and place the final implant.
This two-stage approach is less invasive than flap reconstruction and usually involves a shorter recovery time.

Ranked a Top Cancer Hospital in Nation
Moffitt is ranked 15th in the nation and is the top-ranked cancer hospital in Florida and the Southeast in Newsweek’s “America’s Best Cancer Hospitals."
Flap (Autologous Tissue) Reconstruction
Also known as autologous reconstruction, this approach uses tissue from another area of the body to recreate the breast shape. Many patients feel this option provides a more natural look and feel. Because it uses the patient’s own tissue, flap reconstruction typically does not require an implant.
Flap reconstruction techniques are typically categorized by the donor site used.
Back (Latissimus Dorsi Flap)
This technique uses skin, fat and muscle from the upper back to create a new breast mound. In some cases, an implant or tissue expander may also be placed to achieve the desired volume.
A latissimus dorsi flap reconstruction may be a suitable option for a patient who has previously received radiation therapy or experienced complications from a prior implant-based reconstruction.
Abdomen (TRAM and DIEP Flaps)
The abdomen is one of the most common donor sites for breast reconstruction.
There are several types of abdominal tissue flap breast reconstruction, including:
- Transverse rectus abdominis muscle (TRAM) flap – Uses skin, fat and a portion of the abdominal muscle to form the breast mound
- Muscle-sparing free TRAM – Uses only a small portion of abdominal muscle to help maintain the structure and strength of the abdomen
- Deep inferior epigastric perforator (DIEP) flap – Preserves the abdominal muscle, potentially reducing the risk of surgical complications and recovery time
Thigh (TUG and PAP Flaps)
If the patient is very thin or has had prior abdominal surgery, the tissue needed for breast reconstruction may be taken from the thighs. The two main types of thigh flap breast reconstruction are:
- Transverse upper gracilis (TUG) flap – Uses tissue and a small portion of the gracilis muscle from the inner thigh
- Profunda artery perforator (PAP) flap – Uses skin and fat from the upper thigh or buttock crease to minimize visible scarring
The surgical team will help determine which reconstruction approach is most appropriate based on the patient’s overall health, cancer treatment plan and desired outcome.
Who is a Good Candidate for Breast Reconstruction Surgery?
In general, breast reconstruction surgery may be suitable for a patient who:
- Is planning to undergo (or has already undergone) a mastectomy or lumpectomy
- Is in good overall health and able to tolerate surgery
- Has realistic expectations about the outcome of the procedure
- Has no known medical conditions that could impair healing, such as uncontrolled diabetes
- Does not smoke
To determine whether the patient is a good candidate for breast reconstruction surgery and, if so, the most appropriate technique, the physician will evaluate several factors, including the patient’s medical history, cancer treatment plan and personal goals.
What are the Benefits of Breast Reconstruction Surgery?
For a patient who chooses to undergo breast reconstruction surgery, the procedure offers several potential benefits, including:
- Improved breast shape and symmetry
- Better clothing fit without the need for an external prosthesis
- Enhanced self-esteem and body confidence
- A sense of physical and emotional closure following breast cancer treatment
How to Prepare for Breast Reconstruction Surgery
Before breast reconstruction surgery, the physician will review the patient’s medical history, evaluate imaging studies and discuss the overall treatment plan. The patient may be advised to pause certain medications or supplements to help minimize the risk of bleeding. If the patient smokes, quitting before surgery can greatly reduce the likelihood of complications and support better healing. Maintaining a healthy diet and engaging in regular, physician-approved physical activity can also promote a safe procedure and smooth recovery.
 The Only Florida-based NCI-designated Comprehensive Cancer Center
The Only Florida-based NCI-designated Comprehensive Cancer Center
Recognized for its scientific excellence, Moffitt is the only National Cancer Institute-designated Comprehensive Cancer Center based in Florida.
What to Expect After Breast Reconstruction Surgery
Immediately after breast reconstruction surgery, the patient will spend some time in the hospital while the healthcare team monitors the initial healing process. Recovery time can vary depending on the type of procedure performed. While recovery from an implant-based reconstruction typically takes a few weeks, full healing after a flap reconstruction can take several weeks to a few months.
The surgeon will provide detailed postoperative instructions, including guidance on incision care, pain management and when to resume normal activities. In some cases, additional surgery may be considered later to refine the shape or symmetry of the breast.
What are the Risks and Potential Complications of Breast Reconstruction Surgery?
As with any surgical procedure, breast reconstruction surgery carries certain risks, including:
- Excessive bleeding
- Infection at the incision site
- Changes in breast sensation
- Poor wound healing or scarring
- Implant complications, such as rupture or capsular contracture
- Flap failure (rare)
Before the procedure, the surgical team will fully explain the risks and provide detailed guidance to help manage them.
Benefit from World-Class Care at Moffitt Cancer Center
The highly respected breast surgeons at Moffitt have extensive experience in performing advanced breast reconstruction techniques, combining precision, safety and artistry to achieve natural-looking results.
Our team collaborates closely with medical and radiation oncologists to develop personalized treatment plans, and eligible patients may also have access to innovative therapies through our breast cancer clinical trials.
If you would like to learn more about breast cancer reconstruction, you are welcome to talk with a specialist in our highly acclaimed Don & Erika Wallace Comprehensive Breast Program. At Moffitt, we understand that breast reconstruction is more than a medical decision—it is also a personal one. Our compassionate team will guide you through every step, helping you make a choice that feels right for you.
To request an appointment, call 1-888-663-3488 or submit a new patient registration form online. We do not require referrals.
