Radiation Therapy for Meningioma
Meningioma is a type of tumor that develops in the protective membranes that surround the brain and spinal cord. Most meningiomas are noncancerous (benign), but a small percentage are atypical or cancerous (malignant), which means they may grow more aggressively and potentially spread to nearby tissues or distant organs.
These intracranial tumors are most commonly found in older adults and occur more frequently in women than men. The exact cause is not fully understood, but genetic mutations, prior radiation exposure and certain rare inherited conditions, such as neurofibromatosis type 2 (NF2), may increase the risk.
Meningioma symptoms can vary depending on the size and location of the tumor. Common signs include headaches, seizures, visual disturbances, hearing loss and behavioral changes. Typically, the diagnostic process involves a clinical assessment and imaging studies, sometimes followed by a biopsy.

Ranked a Top Cancer Hospital in Nation
Moffitt is ranked 15th in the nation and is the top-ranked cancer hospital in Florida and the Southeast in Newsweek’s “America’s Best Cancer Hospitals."
Is meningioma treatable or curable?
Meningiomas are often highly treatable and, in many cases, can be cured—especially when detected early. Even if a cure is not possible, radiation therapy may effectively control the growth of the tumor, reduce the symptoms and improve the patient’s quality of life.
What is radiation therapy?
Radiation therapy uses high-energy beams or particles to damage the DNA inside rapidly dividing cancer cells, preventing the cells from growing and multiplying. Over time, this may cause the tumor to shrink.
Why is radiation therapy used for meningioma?
The primary goal of radiation therapy for meningioma is to destroy or control tumor cells while preserving surrounding healthy tissues. It may be used to:
- Shrink a tumor before surgery to make it easier to remove
- Eliminate cancer cells that remain after surgery to help reduce the risk of recurrence
- Control the growth of a tumor that cannot be safely removed
- Relieve symptoms caused by pressure on nearby structures
For meningioma, radiation therapy may be used as a standalone treatment or in combination with other therapies as part of a comprehensive care plan.
Types of radiation therapy for meningioma
Radiation therapy for meningioma can be delivered in several ways, depending on the type, location and size of the tumor and how close it is to sensitive brain structures. The healthcare team will determine the most appropriate type and technique to target the tumor effectively while protecting nearby healthy tissues. Each approach delivers radiation therapy differently, either from outside the body or inside/near the tumor. Systemic radiation therapy—which uses radioactive drugs (radiopharmaceuticals) that enter the bloodstream and travel throughout the body—is generally not used for meningioma unless part of a clinical trial.
External beam radiation therapy (EBRT)
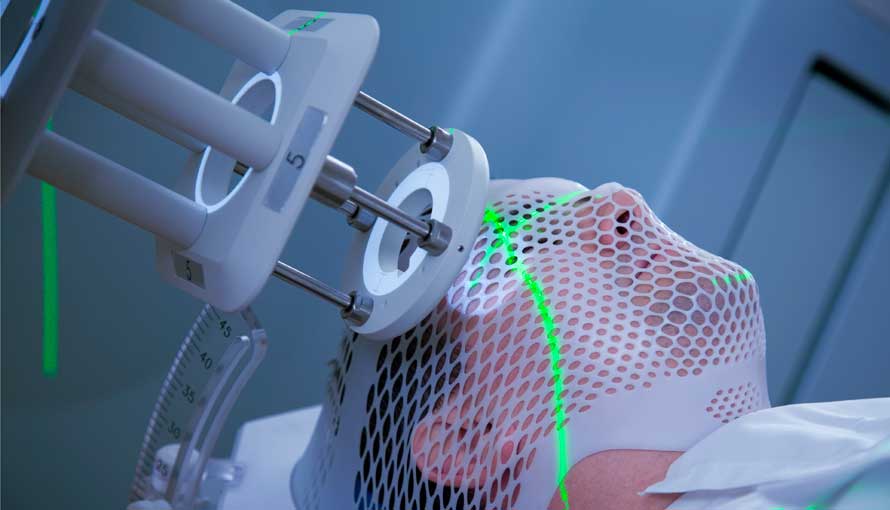
EBRT delivers high-energy beams from an external machine (linear accelerator), precisely targeted at the tumor. Advanced imaging and computer-guided systems can help shape and focus the beams to minimize exposure to healthy tissues.
Common EBRT techniques for meningioma include:
- Intensity-modulated radiation therapy (IMRT) – Delivers powerful radiation beams in varying intensities to conform closely to the shape of the tumor
- Proton radiation therapy – Uses powerful rays made up of protons (rather than traditional ionizing radiation) to destroy abnormal cells
- Stereotactic radiosurgery (SRS) – Provides a single high dose of focused radiation to a small tumor, often in a hard-to-reach area of the body
- Fractionated stereotactic radiotherapy (FSRT) – Divides the radiation dose into several small sessions to treat a large or sensitive tumor
Internal radiation therapy (brachytherapy)
Though used less commonly for meningioma than EBRT, internal radiotherapy may be considered in select cases, often during or after surgery. The treatment involves surgically placing a small radioactive source inside or near the tumor site. Brachytherapy allows for the delivery of a high dose of radiation directly to the tumor while limiting exposure to nearby healthy tissues.


Florida's Top Choice for Cancer Care
Schedule an AppointmentWhat to expect with radiation therapy for meningioma
EBRT for meningioma involves several carefully planned steps to ensure the treatment is delivered safely, accurately and effectively. By understanding the process, the patient can set expectations and gain confidence about the treatment. Each phase—from preparation and delivery to follow-up and recovery—is designed to achieve the best possible outcome while maintaining comfort and well-being.
Before radiation therapy for meningioma
Before starting EBRT, the patient will meet with a team of specialists, including radiation oncologists, neurosurgeons, nurses and other medical professionals. Preparation typically includes:
- A consultation and evaluation – The patient will undergo a thorough medical assessment and discuss their treatment goals with the healthcare team.
- A simulation session – Imaging studies, such as computed tomography (CT), magnetic resonance imaging (MRI) or positron emission tomography (PET) scans, can help the team map the tumor and surrounding tissues.
- Immobilization devices – Custom molds, masks or cushions may be created to help keep the patient positioned properly during each session.
- Treatment plan creation – Medical physicists and dosimetrists will work closely with the radiation oncologist to calculate the safest and most effective radiation dose.
During radiation therapy for meningioma
EBRT is typically given five days per week over several weeks. On each treatment day:
- The patient will check in at the treatment center and change into a gown
- A radiation team member will position the patient comfortably and correctly on the treatment table
- While the patient is monitored continually through cameras and microphones, the linear accelerator will deliver energy beams painlessly within minutes.
Each session usually lasts 15 to 30 minutes, and the patient can go home immediately afterward.
Possible side effects of radiation therapy for meningioma
The side effects of EBRT can vary depending on the total dose and the patient’s response. Most are temporary, manageable and localized to the treated area. The healthcare team can provide strategies to minimize any discomfort, and the patient should report any new or worsening symptoms promptly.
Common side effects of radiation therapy for meningioma include:
- Fatigue – A general feeling of tiredness that may increase during treatment
- Hair thinning or loss – May occur in the area of the scalp where the radiation beam is focused
- Skin irritation – Redness, dryness or tenderness similar to a sunburn
- Headaches or scalp tenderness – May develop if the treated area becomes temporarily inflamed or irritated by the radiation
- Nausea – Can occur if the radiation affects the chemoreceptor trigger zone (CTZ) or the vomiting center, both of which are located in the brainstem
Though not often seen, long-term or late-onset side effects of radiation therapy for meningioma may include:
- Cognitive changes – Mild memory or concentration difficulties
- Hormonal imbalances – Can develop if the pituitary gland is affected by the radiation
- Radiation necrosis – Damage to brain tissue near the treatment site (highly uncommon)
- Secondary tumor risk – Exceedingly rare but possible with long-term radiation exposure
Managing daily life during radiation therapy for meningioma
Maintaining a normal daily routine during radiation therapy is an important part of promoting overall health and well-being. Simple adjustments to diet, activity levels and self-care habits can minimize any side effects and support recovery. The healthcare team can provide guidance tailored to the patient’s needs, aiming to preserve strength, manage fatigue and enhance comfort throughout treatment. Helpful tips include:
- Nutrition – Eat balanced meals rich in protein and nutrients to support healing.
- Skin care – Wash with gentle, fragrance-free cleansers and avoid using harsh lotions in the treated area.
- Physical activity – Maintain a light exercise program, such as walking or cycling, to help reduce fatigue.
- Infection prevention – Wash hands often and avoid exposure to illness (radiation therapy can temporarily weaken the immune system).
- Emotional health – Manage stress or anxiety with the help of a support group or counselor.
Follow-up care and monitoring after radiation therapy for meningioma
After radiation therapy, regular follow-up visits and imaging scans can help the healthcare team monitor the patient’s progress, assess the treatment response and manage any side effects. Long-term monitoring will remain important because meningioma can potentially recur years later.
Benefit from world-class care at Moffitt Cancer Center
Moffitt offers the latest radiation delivery techniques and technologies, a robust portfolio of clinical trials and a strong record of successful outcomes in treating complex meningiomas and brain tumors. While our vast range of leading-edge options enables us to provide each patient with the most appropriate treatment plan, it is the expertise of our multispecialty team that truly sets us apart. Our patient-centered approach emphasizes compassionate, comprehensive care from diagnosis through recovery.
If you would like to learn more about radiation therapy for meningioma, you can request an appointment with a specialist at Moffitt by calling 1-888-663-3488 or submitting a new patient registration form online. We do not require referrals.
Treatment
